Overactive Bladder and Urge Incontinence
Incidence

Overactive bladder (OAB) is defined by urinary urgency – the need to rush to the toilet, and the difficulty in postponing this need. Urinary urgency is often associated with urinary frequency, which occurs during the day and often at night (nocturia). In some patients OAB results in urge urinary incontinence (UUI).
OAB is the most common bladder symptom as you age. In the United Kingdom 17% of the adult population have some degree of OAB symptoms (5.15 million sufferers in the UK) and nearly one-third of retirees report OAB symptoms. One third of women with OAB symptoms are wet.
Symptoms and signs
The degree of OAB symptoms and urge incontinence can vary considerably. For some women the leak is small and is managed by fluid restriction and mapping toilets. Symptoms are often worsened by temperature change and particularly in cold weather. Awareness of near availability of toilet facilities often leads to sudden peaks of urgency most typically when reaching your front door. This is often termed “latchkey incontinence“.Mixed incontinence describes a combination of stress incontinence and urge incontinence symptoms (see Stress Incontinence) and the two causes of urinary leak are often seen together.
Diagnostics
Your doctor will question you on your symptoms and your previous medical, surgical and obstetric history. An examination of your abdomen and pelvis will be a part of this assessment. All examinations are chaperoned by qualified nursing staff. You may be asked to complete questionnaires and fluid charts as part of your assessment. The gold standard investigation to assess incontinence is called an Urodynamic study. This involves the passage of a fine catheter into the bladder and rectum to measure pressures as the bladder fills and empties. The rectal catheter is used to subtract the abdominal pressure to give an accurate bladder reading.
A urodynamic study showing sudden peaks of pressure (pink line) when the bladder contracts during filling. The patient describes significant urgency and urge leakage occurred during these episodes (green line). The peak of the bladder contractions describes the severity of the condition. The urodynamic test is combined with Voiding Cytourethrography – Xray images – in order to get both pressures and pictures of your pelvic floor support (see Stress Incontinence). The urodynamic study takes approximately 30 minutes to perform and is not painful. Your consultant will give further details.
Treatment options
Medical Treatment
There are two types of pills to treat OAB symptoms. For many years anticholinergic pills (or skin patches) have been the only available treatment urgency symptoms. There are a number of different anticholinergic pills available on the market and your consultant will advise you on the most appropriate for you. The most common side effects are dry eyes and dry mouth. There has been recent awareness that anticholinergic pills may affect cognitive function (concentration and memory) in elderly patients or those with impaired function for other reasons. It is important to note that there is no evidence to date that anticholinergic medications are the cause dementia. In 2013 a new class of drugs that treat OAB symptoms – the β3-adrenoceptor agonist – was launched. At present only one medication is available on the UK market. Mirabegron has similar efficacy (benefits) to the anticholinergic medications but a different side-effect profile. Blood pressure monitoring is recommended when the drug is started. Your consultant will advise you on which medication is best for you.
Onabotulinum A Injections (Botox) Treatment


Botulinum toxin is isolated from Clostridium bacterium. The toxin binds to and blocks nerve endings. In low concentrations this causes a temporary ‘relaxation’ of the targeted muscles. Botulinum toxin was initially used medically to treat eye squints and twitches (Strabismus) in the 1980s by relaxing the muscles around the eye. In recent times Botox has been used cosmetically to relax the muscles of the forehead and face and reduce wrinkling. Botulinum toxin can be injected into the bladder wall to block nerve endings and relax the bladder (Detrusor) muscle (see VIDEO BELOW). Botox improves symptoms in approximately two thirds of patients and on average lasts 6 to 9 months (ie needs repeated twice per year). However, over-paralysis of the bladder can lead to difficulty in passing urine. 1-5% (1 in 20) patients require to use in-out catheters temporarily until the Botox effect wears off. The LUS has dedicated nurses who teach all patients who may require to use catheters. More information about Botox can be found via the BAUS leaflets at BAUS and downloading the leaflet on Botulinum toxin A (Botox®) injections into the bladder wall in the Cystoscopy with Other Procedures section.
Percutaneous tibial nerve stimulation
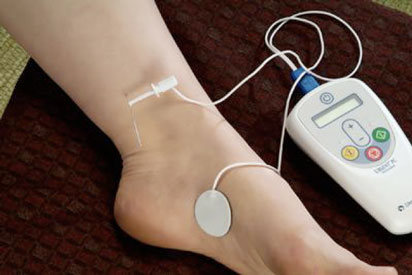
OAB is caused by malfunction of the nerves that control bladder relaxation. These nerves originate from the spine and exit as four nerve roots that exit the base of the spine called the sacrum. The third sacral nerve is the major contributor to bladder control. This nerve root also sends a branch down the leg to the foot. This is called the tibial nerve. Percutaneous tibial nerve stimulation (PTNS) uses electo-acupuncture techniques to pulse stimulate this nerve. Nerve activity is modulated and the bladder is ‘relaxed’. PTNS is performed as weekly sessions and response rates are 47-56%.
Sacral Nerve Stimulation


In sacral neuromodulation the electrical lead (wire) is implanted directly into the third nerve root under X-ray guidance under a short anaesthetic. The lead is initially attached to an external battery, which is worn on a belt for a three-week testing period. If unsuccessful the lead can be removed under a second short anaesthetic. However, if successful a permanent implant can be placed under the skin to control the bladder (see photo). Success rates are 60-70%. The “bladder pacemaker” works for 5 years. Testing phase under anaesthetic where the correct nerve is identified and electrical stimulation causes reflexes making the toe bend and the anus contract.
More information about Sacral Nerve Stimulation (Neuromodulation) can be found via the BAUS leaflets at BAUS and downloading the leaflet on Sacral Nerve Stimulation (Neuromodulation)
Augmentation Cystoplasty

In patients with the most intractable symptoms, an operation can be performed to enlarge (augment) the bladder using a short piece of the small bowel (see diagram). This is very effective in controlling OAB particularly particularly in patients with resistant urge incontinence. However, bladders that have been enlarged with bowel are not able to contract and in most patients do not empty. Patients therefore trade incontinence for dryness, but (intermittent in-out) catheter dependency. More information about augmentation cystoplasty can be found via the BAUS leaflets at BAUS and downloading the leaflet on Enlargement of the Bladder with a piece of bowel (enterocystoplasty)

